Male fertility
Tests and treatments for male reproductive function
About 50% of couples experiencing reproductive difficulties face a male factor in infertility, yet men are less likely to seek fertility evaluation. This is often due to the mistaken belief that male infertility is linked to impotence or loss of masculinity. In reality, timely diagnosis is crucial for identifying the causes and selecting the most appropriate treatment. Male infertility can result from genetic factors, past illnesses, injuries, medications, as well as lifestyle choices. These factors can affect the production or release of sperm and make achieving pregnancy more difficult.

Center for male infertility treatment
The New Life Center assists men with abnormal semen analysis, those needing cryopreservation, as well as couples facing unexplained infertility or unsuccessful IVF attempts. We apply the Israeli model of treatment, based on many years of experience and scientific advancements in reproductive medicine.
Our team is trained in leading Israeli clinics and works under the guidance of world-renowned experts – Prof. Neri Laufer and Dr. Anat Safran. We also serve international patients, thanks to the excellent language skills of our staff.
We are equipped with modern technology, including high-end micromanipulation equipment and specialized incubators that provide optimal conditions for embryos. We also have emergency power backup for complete safety.
We never give up on difficult cases — we take an individualized approach to each patient, combining professionalism with compassionate care. For us, every patient matters, and every story is personal.
Causes of male infertility
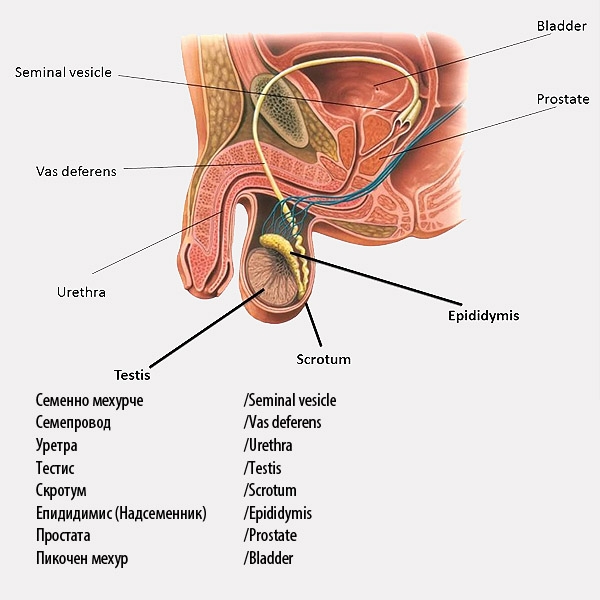
Impaired spermatogenesis
Spermatogenesis — the process of sperm maturation — takes place in the testes and epididymis. Trauma, structural abnormalities, or hormonal disorders can disrupt this process. Evaluation includes physical examination, hormonal testing, and semen analysis (spermogram).
Key parameters in the spermogram:
| Parameter | Normal Range | Abnormality |
|---|---|---|
| Volume | 2–6 ml | Hypospermia |
| Concentration | ≥ 20 million/ml | Oligozoospermia |
| Motility | ≥ 50% | Asthenozoospermia |
| Morphology | ≥ 14% | Teratozoospermia |
(According to WHO standards. For an accurate diagnosis, 2–3 tests are performed at intervals of 6 weeks.)
In about 0.5% of men, spermatogenesis is severely reduced (non-obstructive azoospermia). In such cases, the TEFNA technique is used to retrieve sperm for ICSI fertilization.
Varicocele
About 15% of men have enlarged veins in the scrotum, which increases temperature and disrupts spermatogenesis. It is diagnosed through examination and often leads to reduced fertility.
Impaired sperm transport
After maturation, sperm are transported through the epididymis, vas deferens, and ejaculatory duct. Obstruction along this pathway (including after vasectomy or congenital absence of the vas deferens—often associated with cystic fibrosis) can lead to:
-
Azoospermia – absence of sperm
-
Aspermia – absence of seminal fluid
In such cases, sperm retrieval is performed using methods like PESA, MESA, and TESA, which are also used in ICSI fertilization.
Overall health and lifestyle
Neurological disorders (e.g., spinal cord injuries, multiple sclerosis), sexual dysfunctions, and chronic conditions such as diabetes, hypertension, heart disease, and anemia affect fertility. Additionally:
-
Use of steroids, drugs, and alcohol
-
Unhealthy diet
-
Exposure to toxins
Fertility is a reflection of overall male health.
Consultations
Urologist
Recommended for abnormalities in sperm parameters or infections. The urologist prescribes treatment or additional tests and, if needed, supplements to improve spermatogenesis.
Endocrinologist
Suitable for hormonal imbalances or elevated BMI that may affect fertility.
Psychologist
Prolonged infertility can lead to emotional stress. Our psychologist supports patients dealing with anxiety, guilt, loss, and relationship tension.
Sexologist
Sexual dysfunction is common but often unspoken. Discreet consultations with a sexologist can help restore confidence and intimacy.
Tests

Initial assessment
Evaluation of male fertility begins with a detailed reproductive history and semen analysis review.
Reproductive history includes:
- Past illnesses (e.g., mumps), injuries, or surgeries in the genital area
- Hormonal disorders, puberty abnormalities
- Chronic diseases (diabetes, hypertension), allergies
- Harmful habits (smoking, drugs), physical activity
- Sexual health — infections, erectile dysfunction, etc.
- Exposure to toxic substances
- Duration of infertility and family history
After the history is taken, the doctor may order additional tests.
Semen tests
Semen analysis evaluates the parameters of the seminal fluid. Due to natural fluctuations, at least two samples taken 6 weeks apart are required.
- Samples can be collected at the clinic or at home (delivery within 30 minutes).
- Sexual abstinence of 2–5 days before sampling is recommended.
- If no sperm are found in the ejaculate, surgical retrieval methods such as PESA, MESA, or TESA are used.
When starting an IVF procedure, a fresh sample is taken on the day of egg retrieval or a frozen sample is used.
Hormonal tests
Ordered if semen analysis shows abnormalities. Main hormones tested include:
- FSH (Follicle Stimulating Hormone)
- LH (Luteinizing Hormone)
- Testosterone
Additional tests may include hormones from the hypothalamus, pituitary gland, and adrenal glands.
Genetic tests
Recommended in cases of:
- Azoospermia (complete absence of sperm)
- Genital anomalies (e.g., absence of vas deferens)
- Multiple spontaneous miscarriages in the family
New technologies
Assisted reproduction is one of the most rapidly evolving fields in medicine. At the New Life Male Center, we apply innovative technologies that improve success rates even in complex cases of male infertility.
Computer-assisted sperm analysis (CASA)
CASA is an automated system that precisely evaluates:
- Sperm concentration, motility, and morphology
- Speed and trajectory of movement
- Head, neck, and tail dimensions
The advantage of CASA is its objectivity — results are not influenced by human error. The software generates detailed graphs and images, making the analysis more informative and easier to interpret.
IMSI fertilization
IMSI (Intracytoplasmic Morphologically Selected Sperm Injection) is an advanced form of ICSI where sperm are examined under high magnification (up to x6000).
This allows for the precise selection of the most morphologically healthy sperm, increasing the chances of successful fertilization. IMSI is recommended for:
- Severe male factor infertility
- Very low percentage of normal morphology
- Repeated unsuccessful IVF cycles
Testicular biopsy (TEFNA)
Used in men with azoospermia when obstruction is suspected but spermatogenesis is preserved. At New Life, we perform the minimally invasive TEFNA technique:
- A fine needle with an attached syringe is inserted into the testis
- Multiple areas are biopsied with minimal tissue damage
- Retrieved sperm can be used for ICSI fertilization
